Volume 8, Issue 1 (1-2020)
J. Pediatr. Rev 2020, 8(1): 53-58 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Akbari H, Ghahremani-Chabok A, Mousavi S A. Inadvertent Subcutaneous Injection of Atracurium During Circumcision Operation. J. Pediatr. Rev 2020; 8 (1) :53-58
URL: http://jpr.mazums.ac.ir/article-1-234-en.html
URL: http://jpr.mazums.ac.ir/article-1-234-en.html
1- Department of Anesthesiology, School of Medicine, Mazandaran University of Medical Sciences, Sari, Iran , hooshangakbari48@yahoo.com
2- Department of anesthesiology, School of Paramedicine, Mazandaran University of Medical Sciences, Sari, Iran
3- Department of Pediatric, School of Medicine, Mazandaran University of Medical Sciences, Sari, Iran
2- Department of anesthesiology, School of Paramedicine, Mazandaran University of Medical Sciences, Sari, Iran
3- Department of Pediatric, School of Medicine, Mazandaran University of Medical Sciences, Sari, Iran
Full-Text [PDF 468 kb]
(3386 Downloads)
| Abstract (HTML) (8288 Views)
Investigation of the causes of this medical error revealed that errors occurred at the stage of drug dispensing and administering. Inattention was noted in the nurse anesthetist who placed the potentially lethal drug such as atracurium in an inappropriate place and the nurse who administered the wrong medication. Furthermore, errors also arose from the perinatal clinic’s failure to establish secure medical procedures to safeguard patients’ safety. Their results demonstrated that medication errors could threaten patients’ lives, lead to mental or physical injuries, and family stress. Policies to prevent such medication errors can be emphasizing the education of medical practitioners, improving distribution and implementation of practice guidelines, and developing better mechanisms for identifying negligent behavior and introducing appropriate disciplinary actions.
However, previous case studies of atracurium overdose in infants was associated with minimal clinical responses (9). Durcan and Carter reported a dose of 5.1mg/kg atracurium via intravenous bolus injection on a three-week-old infant, who manifested by skin flushing, hypotension, and tachycardia, but the symptoms subsided after medical management (10). Charlton et al. also reported skin flushing at a dose of 37 mg atracurium over 75 min in a two-month-old infant (11).
Minimizing medication errors and improving injection safety are the most important and essential parts of anesthesiology and medical process (1, 12). As suggested by Jensen et al., the syringe label should be read carefully before administration to reduce the prevalence of medication errors, which is one of the important aspects of patient’s safety (13). Kothari et al. have reviewed the incidence, types, risk factors, and preventive measures of the medication errors in anesthesia and critical care and concluded that vigilance and attention, standardized protocol, and ‘think before act’ are the key factors to avoid an occurrence of medication errors (6).
Inadvertent drug injection causes serious adverse effects such as systemic problems, gangrene, limb ischemia, and necrosis that were causing permanent damage, dysfunction, paresthesia, and even cardiac arrest (3, 14). Also, economic consequences such as losing productivity, requires a lengthy rehabilitation, care, and follow-up. Recommendations for the treatment of complications are mainly experimental and based on the treatment of any complications, rehabilitation, and symptom relief (15, 16).
Atracurium, is an amino steroid, non-depolarizing muscle relaxant, whose intravenous injection causes skeletal muscle relaxation, including respiratory muscles. About 3 minutes after intravenous injection, respiratory apnea begins, and the patient needs respiratory support. Atracurium is recommended to be used only by intravenous route (4). The use of atracurium in therapeutic doses harms blood pressure and cardiovascular system, but it may cause histamine release, and there is a risk of allergic reactions. Atracurium is degraded through Hoffman elimination. Body pH and temperature are important parts of Hoffman system for atracurium metabolism (4, 14).
Bradycardia occurs in children under the age of 14 years. This problem is attributed to the high incidence of airway events in which hypoxemia is associated with rapid deterioration in heart rate. Atropine is recommended as a second-line agent in refractory asystole or the initial management of bradycardia associated with hypotension. This issue is important because aggressive resuscitation of the cardiovascular system may follow an episode of hypoxemia, and the possibility of multiple causes for bradycardia will always need to be considered (17).
According to the studies, inadvertently intrathecal injection of atracurium causes signs and symptoms such as tachycardia, hypotension, and diplopia (18, 19). However, two cases of inadvertently intrathecal injection of atracurium have been reported that did not show hemodynamic symptoms and complications (20, 21). According to reports, high-dose intravenous injection of atracurium causes seizure (19). Also, it has been reported that intra-arterial injection of atracurium causes marked ischemic appearance which is resolved with sympatholytic caudal block (22).
In our case, about five minutes after subcutaneous injection for local anesthesia, the patient developed respiratory apnea, cyanosis, muscle relaxation, and bradycardia and after taking supportive and therapeutic cares, there was no complication. The patient was discharged after complete recovery without any problems.
In this case report, a two-month-old infant developed symptoms and respiratory problems following inadvertently subcutaneous injection of atracurium instead of lidocaine for local anesthesia, for circumcision (Figure 2). After receiving respiratory support, the patient was transferred to the NICU for taking supportive and therapeutic cares and be under follow up. Finally, the patient, after complete recovery, was discharged without any problems or complication. According to the literature, this is the first report of inadvertently subcutaneous injection of atracurium for circumcision.
4. Conclusion
Medication errors can endanger patients’ lives, cause respiratory or other problems, and worries families. This case report highlights the importance of the immediate establishment of ventilation and perfusion in the field after the inadvertent administration of atracurium. Strategies to prevent such medication errors are emphasizing the education of medical practitioners, improving dissemination and enforcement of practice guidelines, and developing better mechanisms for identifying negligent behavior and instituting appropriate disciplinary actions. Also, important drugs should be made in different colors.
Ethical Considerations
Compliance with ethical guidelines
Our study observed the ethical principles outlined in the Declaration of Helsinki as amended in 2013. Written consent was obtained from the patient’s family to access the details of the case and to publish the results.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors..
Authors contribution's
Conceptualization, study design, writing the manuscript, review of data, and critical revision of the manuscript for relevant intellectual content: Hooshang Akbari and Seyed Abdollah Mousavi; and Reviewing the databases: Anahita Ghahremani Chabok.
Conflicts of interest
The authors declared no conflict of interest.
References
Full-Text: (5342 Views)
1. Introduction
Inadvertent drug injection is one of the medical errors during treatment procedures, which causes complications. Medication errors due to the type of drug administered, dosage, amount of administration, or site of administration, cause various complications and symptoms (1). Inadvertent drug injection can cause extensive and irreversible side effects (2, 3).
Atracurium is a Neuromuscular Relaxant (NMR) and anesthetic drug. After systemic absorption of the drug, the patient needs to receive respiratory support (4). Circumcision in infants is usually done under local anesthesia with subcutaneous injection of lidocaine. We report a case of inadvertent subcutaneous injection of atracurium for circumcision and then briefly review the international databases related to the reported case.
2. Case Presentation
A 2-month-old infant was scheduled for circumcision under local anesthesia. The surgeon suggested 15mg of lidocaine 1% be prepared for local anesthesia. The drug was prepared by the operating room technician and injected by the surgeon around the infant’s penis to the amount of 15mg. After five minutes, the infant developed bradycardia, respiratory distress, cyanosis, muscle relaxation, and decreased oxygen saturation. Cardiopulmonary resuscitation and intubation were immediately started. With symptoms development, the operation was discontinued, and the infant was intubated (Cuffless N3 ETT) and connected to the mechanical ventilation machine with pressure mode. After IV line insertion with blue angiocath, atropine 100μg was injected for treating bradycardia. Then the search was conducted to find the cause of bradycardia and apnea. After a while, it became clear that atracurium, instead of lidocaine, was injected inadvertently. Two hours after atropine injection, intubation, and stabilizing the infant’s condition, he was transferred to the neonatal intensive care unit (NICU) in another center to maintain respiratory support and receive supportive care.
On arrival, the infant’s vital signs were as follows: HR=125 and SPO2=93%. After 30 minutes, Arterial Blood Gas ABG, liver tests, and blood serum tests were done, whose results were normal. About 8 hours later, the infant got agitated, and extubation was done. Because of O2 saturation of 98%, lack of respiratory distress, good consciousness, and normal blood gas test, re-intubation was not done. To control and monitor the symptoms, the infant was kept under follow up in the NICU for two days and then the child was transferred to the Pediatrics General Department. In the Pediatric Department, the symptoms such as fever, crackles, O2 saturation below 90% and opacity in chest X-ray were reported, and the risk of aspiration was raised. As a result, antibiotic therapy with ceftriaxone and clindamycin was started for him for a week. After a full recovery, he was discharged without any problem or complication.
3. Discussion and Review of Literature
Medication errors are common in the health care system and reported to be the seventh most common cause of death overall (5). One of the medication errors may be attributed to drugs prepared in syringes for injection, and the risk of this kind of mistakes in the operation room is high (6). Lots of medication errors are caused by ampoules or syringes that have similar size, label, or color. Other factors include drug location, lack of proper labeling, and inaccuracy in equipment selection. Significant factors in medication errors are ‘fatigue’ and ‘inattention’ (2, 3).
In an Australian study, ‘fatigue’ and ‘inattention’ were reported respectively as the causes of 10% and 50% of all medication errors (7). Improper labeling is another reason for medication errors in anesthesiology drugs. Strategies described to prevent such mistakes include clear fonts for labeling, emphasizing the generic name of drugs, and using a two-person check (2).
Iwashaki H reported neuromuscular effects of subcutaneous administration of pancuronium in a 67-year-old man who underwent surgery for removal of brain tumor under enflurane anesthesia. After insertion of 18G Teflon catheter into a peripheral vein on the ankle, 6 mg bolus dose of pancuronium was administered through this catheter. Shortly after the administration, a swelling was noticed around the site of the venous catheter. About 40 min after the administration of pancuronium, no response to peripheral nerve stimulation was detected. Accidental subcutaneous injection of pancuronium was assumed. The patient’s trachea was extubated 6 hours after pancuronium administration. Neuromuscular function was monitored continuously by peripheral nerve stimulator in the recovery room. No sign of complication was reported during the recovery period (8).
In an Iranian study, Nasiri et al. evaluated unwanted errors in anesthesia and related factors in Mazandaran Province hospitals and concluded that medication errors were potential risk factors during anesthesia and health care. Following medication protocols, detailed drug monitoring (by two persons before injection), a quiet and orderly environment, and planning for recording and reporting any error were their suggestions for reducing and preventing anesthesia mistakes (1).
Wu-Shiun Hsieh et al. (2006) reported seven newborns (Cases A, B, C, D, E, F, and G) who were involved in the medical accident of atracurium injection at ages of four to five days in a local perinatal clinic in Taipei, Taiwan.
In Taiwan, the hepatitis B vaccination is obligatory for newborns before hospital discharge. The newborns in the perinatal clinic were scheduled to receive hepatitis B vaccination on the fourth or fifth day after birth. In this clinic, the muscle relaxant atracurium was kept in the same refrigerator beside the hepatitis B vaccine in the nursery. Because the operating room is situated on the same floor as the nursery, the nurse anesthetist placed atracurium in the refrigerator that stored the hepatitis B vaccine. Although the two drugs were provided by different companies and had no similarity in packages, vials, and labels, a nurse in the nursery misidentified the muscle relaxant for the vaccine and sequentially administered one mL (ten mg, equivalent to 2.6-3.3mg/kg) of atracurium intramuscularly to seven newborns. Within minutes of the inadvertent injection, the newborns developed apnea, bradycardia, and cyanosis. Cardiopulmonary resuscitation was immediately started.
All the newborns were subsequently transferred to different hospitals for primary emergency care due to insufficient ventilators and absence of reference hospital. Due to prolonged arrival time, all the newborns in the emergency department became apneic and flaccid. Case A had mild hypotension; case F had bradycardia and unmeasurable blood pressure, and case G was pulseless. A combination of respiratory acidosis and metabolic acidosis were identified in four cases of A, E, F, and G and mild respiratory alkalosis in case D, which might be related to blood sampling after using Ambu bag or ventilator therapy. Hyperglycemia was observed in all cases and a borderline elevation of creatine kinase level in five cases. Treatment was started by intravenous administration of sodium bicarbonate, epinephrine, and dopamine.
Neostigmine and atropine were subsequently administered as antidotes after identifying atracurium as the target injection drug. Unfortunately, resuscitation was unsuccessful in one case, and the patient ultimately died due to multiple organs failure. The remaining survived infants underwent mechanical ventilation (mean duration 26.7h, range: 5-96h), oxygen therapy (mean duration: 3.3 days, range: 2-6 days) and hospitalization (mean duration: 9.8 days, range: 7-12 days). During hospitalization, the echocardiographic and renal ultrasonographic examinations were performed for the newborns. Mild tricuspid regurgitation in two cases, patent foramen ovale and arrhythmia in case F, and normal findings in three cases were revealed in the echocardiographic examination.
The renal ultrasonographic examination results showed poor cortico-medullary differentiation over the upper pole of the right kidney suggesting acute renal failure only in one case. The EEG examinations were normal in three cases, and paroxysmal discharge with diffuse low voltage slow waves, focal spike waves at right temporal-parietal areas, and focal spike waves at right central-parietal areas were observed in the three remaining cases.
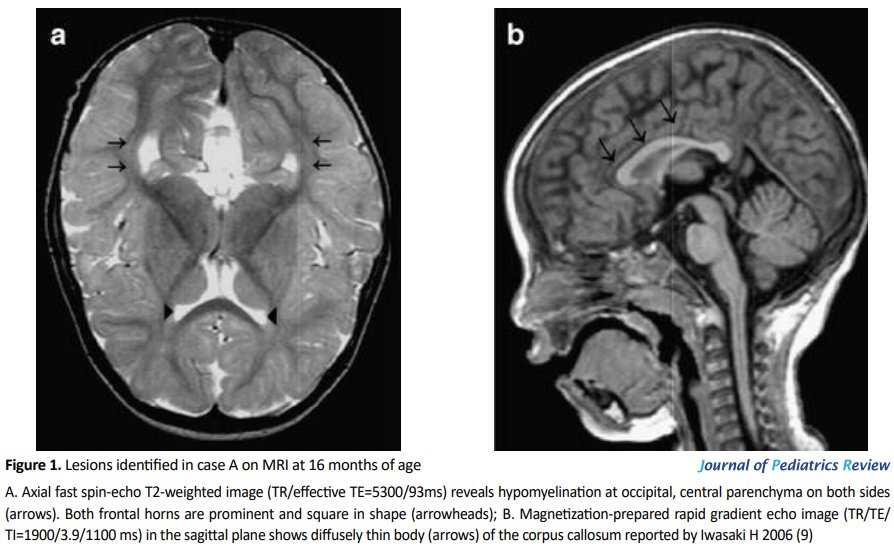
Brain MRI performed at 16 months of age illustrated abnormalities in two cases. One case showed ventricular enlargement, mild hypomyelination at bilateral parietal and occipital central white matter (Figure 1 a) and diffusely thin body of the corpus callosum (Figure 1 b), and another manifested mild hypomyelination at bilateral parietal and occipital central white matter (Figure 1 a, 1 b).
Inadvertent drug injection is one of the medical errors during treatment procedures, which causes complications. Medication errors due to the type of drug administered, dosage, amount of administration, or site of administration, cause various complications and symptoms (1). Inadvertent drug injection can cause extensive and irreversible side effects (2, 3).
Atracurium is a Neuromuscular Relaxant (NMR) and anesthetic drug. After systemic absorption of the drug, the patient needs to receive respiratory support (4). Circumcision in infants is usually done under local anesthesia with subcutaneous injection of lidocaine. We report a case of inadvertent subcutaneous injection of atracurium for circumcision and then briefly review the international databases related to the reported case.
2. Case Presentation
A 2-month-old infant was scheduled for circumcision under local anesthesia. The surgeon suggested 15mg of lidocaine 1% be prepared for local anesthesia. The drug was prepared by the operating room technician and injected by the surgeon around the infant’s penis to the amount of 15mg. After five minutes, the infant developed bradycardia, respiratory distress, cyanosis, muscle relaxation, and decreased oxygen saturation. Cardiopulmonary resuscitation and intubation were immediately started. With symptoms development, the operation was discontinued, and the infant was intubated (Cuffless N3 ETT) and connected to the mechanical ventilation machine with pressure mode. After IV line insertion with blue angiocath, atropine 100μg was injected for treating bradycardia. Then the search was conducted to find the cause of bradycardia and apnea. After a while, it became clear that atracurium, instead of lidocaine, was injected inadvertently. Two hours after atropine injection, intubation, and stabilizing the infant’s condition, he was transferred to the neonatal intensive care unit (NICU) in another center to maintain respiratory support and receive supportive care.
On arrival, the infant’s vital signs were as follows: HR=125 and SPO2=93%. After 30 minutes, Arterial Blood Gas ABG, liver tests, and blood serum tests were done, whose results were normal. About 8 hours later, the infant got agitated, and extubation was done. Because of O2 saturation of 98%, lack of respiratory distress, good consciousness, and normal blood gas test, re-intubation was not done. To control and monitor the symptoms, the infant was kept under follow up in the NICU for two days and then the child was transferred to the Pediatrics General Department. In the Pediatric Department, the symptoms such as fever, crackles, O2 saturation below 90% and opacity in chest X-ray were reported, and the risk of aspiration was raised. As a result, antibiotic therapy with ceftriaxone and clindamycin was started for him for a week. After a full recovery, he was discharged without any problem or complication.
3. Discussion and Review of Literature
Medication errors are common in the health care system and reported to be the seventh most common cause of death overall (5). One of the medication errors may be attributed to drugs prepared in syringes for injection, and the risk of this kind of mistakes in the operation room is high (6). Lots of medication errors are caused by ampoules or syringes that have similar size, label, or color. Other factors include drug location, lack of proper labeling, and inaccuracy in equipment selection. Significant factors in medication errors are ‘fatigue’ and ‘inattention’ (2, 3).
In an Australian study, ‘fatigue’ and ‘inattention’ were reported respectively as the causes of 10% and 50% of all medication errors (7). Improper labeling is another reason for medication errors in anesthesiology drugs. Strategies described to prevent such mistakes include clear fonts for labeling, emphasizing the generic name of drugs, and using a two-person check (2).
Iwashaki H reported neuromuscular effects of subcutaneous administration of pancuronium in a 67-year-old man who underwent surgery for removal of brain tumor under enflurane anesthesia. After insertion of 18G Teflon catheter into a peripheral vein on the ankle, 6 mg bolus dose of pancuronium was administered through this catheter. Shortly after the administration, a swelling was noticed around the site of the venous catheter. About 40 min after the administration of pancuronium, no response to peripheral nerve stimulation was detected. Accidental subcutaneous injection of pancuronium was assumed. The patient’s trachea was extubated 6 hours after pancuronium administration. Neuromuscular function was monitored continuously by peripheral nerve stimulator in the recovery room. No sign of complication was reported during the recovery period (8).
In an Iranian study, Nasiri et al. evaluated unwanted errors in anesthesia and related factors in Mazandaran Province hospitals and concluded that medication errors were potential risk factors during anesthesia and health care. Following medication protocols, detailed drug monitoring (by two persons before injection), a quiet and orderly environment, and planning for recording and reporting any error were their suggestions for reducing and preventing anesthesia mistakes (1).
Wu-Shiun Hsieh et al. (2006) reported seven newborns (Cases A, B, C, D, E, F, and G) who were involved in the medical accident of atracurium injection at ages of four to five days in a local perinatal clinic in Taipei, Taiwan.
In Taiwan, the hepatitis B vaccination is obligatory for newborns before hospital discharge. The newborns in the perinatal clinic were scheduled to receive hepatitis B vaccination on the fourth or fifth day after birth. In this clinic, the muscle relaxant atracurium was kept in the same refrigerator beside the hepatitis B vaccine in the nursery. Because the operating room is situated on the same floor as the nursery, the nurse anesthetist placed atracurium in the refrigerator that stored the hepatitis B vaccine. Although the two drugs were provided by different companies and had no similarity in packages, vials, and labels, a nurse in the nursery misidentified the muscle relaxant for the vaccine and sequentially administered one mL (ten mg, equivalent to 2.6-3.3mg/kg) of atracurium intramuscularly to seven newborns. Within minutes of the inadvertent injection, the newborns developed apnea, bradycardia, and cyanosis. Cardiopulmonary resuscitation was immediately started.
All the newborns were subsequently transferred to different hospitals for primary emergency care due to insufficient ventilators and absence of reference hospital. Due to prolonged arrival time, all the newborns in the emergency department became apneic and flaccid. Case A had mild hypotension; case F had bradycardia and unmeasurable blood pressure, and case G was pulseless. A combination of respiratory acidosis and metabolic acidosis were identified in four cases of A, E, F, and G and mild respiratory alkalosis in case D, which might be related to blood sampling after using Ambu bag or ventilator therapy. Hyperglycemia was observed in all cases and a borderline elevation of creatine kinase level in five cases. Treatment was started by intravenous administration of sodium bicarbonate, epinephrine, and dopamine.
Neostigmine and atropine were subsequently administered as antidotes after identifying atracurium as the target injection drug. Unfortunately, resuscitation was unsuccessful in one case, and the patient ultimately died due to multiple organs failure. The remaining survived infants underwent mechanical ventilation (mean duration 26.7h, range: 5-96h), oxygen therapy (mean duration: 3.3 days, range: 2-6 days) and hospitalization (mean duration: 9.8 days, range: 7-12 days). During hospitalization, the echocardiographic and renal ultrasonographic examinations were performed for the newborns. Mild tricuspid regurgitation in two cases, patent foramen ovale and arrhythmia in case F, and normal findings in three cases were revealed in the echocardiographic examination.
The renal ultrasonographic examination results showed poor cortico-medullary differentiation over the upper pole of the right kidney suggesting acute renal failure only in one case. The EEG examinations were normal in three cases, and paroxysmal discharge with diffuse low voltage slow waves, focal spike waves at right temporal-parietal areas, and focal spike waves at right central-parietal areas were observed in the three remaining cases.
Brain MRI performed at 16 months of age illustrated abnormalities in two cases. One case showed ventricular enlargement, mild hypomyelination at bilateral parietal and occipital central white matter (Figure 1 a) and diffusely thin body of the corpus callosum (Figure 1 b), and another manifested mild hypomyelination at bilateral parietal and occipital central white matter (Figure 1 a, 1 b).
Investigation of the causes of this medical error revealed that errors occurred at the stage of drug dispensing and administering. Inattention was noted in the nurse anesthetist who placed the potentially lethal drug such as atracurium in an inappropriate place and the nurse who administered the wrong medication. Furthermore, errors also arose from the perinatal clinic’s failure to establish secure medical procedures to safeguard patients’ safety. Their results demonstrated that medication errors could threaten patients’ lives, lead to mental or physical injuries, and family stress. Policies to prevent such medication errors can be emphasizing the education of medical practitioners, improving distribution and implementation of practice guidelines, and developing better mechanisms for identifying negligent behavior and introducing appropriate disciplinary actions.
However, previous case studies of atracurium overdose in infants was associated with minimal clinical responses (9). Durcan and Carter reported a dose of 5.1mg/kg atracurium via intravenous bolus injection on a three-week-old infant, who manifested by skin flushing, hypotension, and tachycardia, but the symptoms subsided after medical management (10). Charlton et al. also reported skin flushing at a dose of 37 mg atracurium over 75 min in a two-month-old infant (11).
Minimizing medication errors and improving injection safety are the most important and essential parts of anesthesiology and medical process (1, 12). As suggested by Jensen et al., the syringe label should be read carefully before administration to reduce the prevalence of medication errors, which is one of the important aspects of patient’s safety (13). Kothari et al. have reviewed the incidence, types, risk factors, and preventive measures of the medication errors in anesthesia and critical care and concluded that vigilance and attention, standardized protocol, and ‘think before act’ are the key factors to avoid an occurrence of medication errors (6).
Inadvertent drug injection causes serious adverse effects such as systemic problems, gangrene, limb ischemia, and necrosis that were causing permanent damage, dysfunction, paresthesia, and even cardiac arrest (3, 14). Also, economic consequences such as losing productivity, requires a lengthy rehabilitation, care, and follow-up. Recommendations for the treatment of complications are mainly experimental and based on the treatment of any complications, rehabilitation, and symptom relief (15, 16).
Atracurium, is an amino steroid, non-depolarizing muscle relaxant, whose intravenous injection causes skeletal muscle relaxation, including respiratory muscles. About 3 minutes after intravenous injection, respiratory apnea begins, and the patient needs respiratory support. Atracurium is recommended to be used only by intravenous route (4). The use of atracurium in therapeutic doses harms blood pressure and cardiovascular system, but it may cause histamine release, and there is a risk of allergic reactions. Atracurium is degraded through Hoffman elimination. Body pH and temperature are important parts of Hoffman system for atracurium metabolism (4, 14).
Bradycardia occurs in children under the age of 14 years. This problem is attributed to the high incidence of airway events in which hypoxemia is associated with rapid deterioration in heart rate. Atropine is recommended as a second-line agent in refractory asystole or the initial management of bradycardia associated with hypotension. This issue is important because aggressive resuscitation of the cardiovascular system may follow an episode of hypoxemia, and the possibility of multiple causes for bradycardia will always need to be considered (17).
According to the studies, inadvertently intrathecal injection of atracurium causes signs and symptoms such as tachycardia, hypotension, and diplopia (18, 19). However, two cases of inadvertently intrathecal injection of atracurium have been reported that did not show hemodynamic symptoms and complications (20, 21). According to reports, high-dose intravenous injection of atracurium causes seizure (19). Also, it has been reported that intra-arterial injection of atracurium causes marked ischemic appearance which is resolved with sympatholytic caudal block (22).
In our case, about five minutes after subcutaneous injection for local anesthesia, the patient developed respiratory apnea, cyanosis, muscle relaxation, and bradycardia and after taking supportive and therapeutic cares, there was no complication. The patient was discharged after complete recovery without any problems.
In this case report, a two-month-old infant developed symptoms and respiratory problems following inadvertently subcutaneous injection of atracurium instead of lidocaine for local anesthesia, for circumcision (Figure 2). After receiving respiratory support, the patient was transferred to the NICU for taking supportive and therapeutic cares and be under follow up. Finally, the patient, after complete recovery, was discharged without any problems or complication. According to the literature, this is the first report of inadvertently subcutaneous injection of atracurium for circumcision.
4. Conclusion
Medication errors can endanger patients’ lives, cause respiratory or other problems, and worries families. This case report highlights the importance of the immediate establishment of ventilation and perfusion in the field after the inadvertent administration of atracurium. Strategies to prevent such medication errors are emphasizing the education of medical practitioners, improving dissemination and enforcement of practice guidelines, and developing better mechanisms for identifying negligent behavior and instituting appropriate disciplinary actions. Also, important drugs should be made in different colors.
Ethical Considerations
Compliance with ethical guidelines
Our study observed the ethical principles outlined in the Declaration of Helsinki as amended in 2013. Written consent was obtained from the patient’s family to access the details of the case and to publish the results.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors..
Authors contribution's
Conceptualization, study design, writing the manuscript, review of data, and critical revision of the manuscript for relevant intellectual content: Hooshang Akbari and Seyed Abdollah Mousavi; and Reviewing the databases: Anahita Ghahremani Chabok.
Conflicts of interest
The authors declared no conflict of interest.
References
- Nasiri E, Padashi S, Nasiri R, Akbari H, Heidari J. [Unwanted errors in Anesthesia and related factors in Mazandaran state hospitals (Persian)]. Journal of Mazandaran University of Medical Sciences. 2015; 25(122):401-6.
- Cooper L, DiGiovanni N, Schultz L, Taylor R, Nossaman B. Human factors contrib-uting to medication errors in anaesthesia practice. American Sociological Association. 2009; 2009:A614.
- Beckers A, Verelst P, Van Zundert A. Inadvertent epidural injection of drugs for in-travenous use. Acta Anæsthesiologica Belgica. 2012; 63(2):75-9. [PMID]
- Della GR, Pompei L, Coccia C, Costa MG, Cecchini V, Vilardi V, et al. Atracurium, cisatracurium, vecuronium and rocuronium in patients with renal failure. Minerva Anestesiologica. 2003; 69(7-8):605-11.
- Stelfox HT, Palmisani S, Scurlock C, Orav EJ, Bates DW. The “To Err is Human” report and the patient safety literature. BMJ Quality & Safety. 2006; 15(3):174-8. [DOI:10.1136/qshc.2006.017947] [PMID] [PMCID]
- Kothari D, Gupta S, Sharma C, Kothari S. Medication error in anaesthesia and criti-cal care: A cause for concern. Indian Journal of Anaesthesia. 2010; 54(3):187-92. [DOI:10.4103/0019-5049.65351] [PMID] [PMCID]
- Webb R, Currie M, Morgan C, Williamson J, Mackay P, Russell W, et al. The Australian incident monitoring study: An analysis of 2000 incident reports. Anaesthesia and Intensive Care. 1993; 21(5):520-8. [DOI:10.1177/0310057X9302100507]
- Iwasaki H, Namiki A, Omote T, Omote K. Neuromuscular effects of subcutaneous administration of pancuronium. Anesthesiology. 1992; 76(6):1049-51. [DOI:10.1097/00000542-199206000-00026] [PMID]
- Hsieh WS, Huang HM, Peng S, Liang JS, Leung C, Yeh GC, et al. Clinical manifestations and neurodevelopmental outcome following an event of accidental intramuscular in-jection of Atracurium in newborns. European Journal of Pediatrics. 2006; 165(6):361-6. [DOI:10.1007/s00431-005-0063-2] [PMID]
- Durcan J, Carter JA. Overdose of atracurium. Anaesthesia. 1986; 41(7):767. [DOI:10.1111/j.1365-2044.1986.tb12868.x] [PMID]
- Charlton AJ, Harper NJN, Edwards D, Wilson AC. Atracurium overdose in a small infant. Anaesthesia. 1989; 44(6):485-6. [DOI:10.1111/j.1365-2044.1989.tb11375.x] [PMID]
- Nwasor E, Sule S, Mshelia D. Audit of medication errors by anesthetists in North Western Nigeria. Nigerian Journal of Clinical Practice. 2014; 17(2):226-31. [DOI:10.4103/1119-3077.127563] [PMID]
- Jensen L, Merry A, Webster C, Weller J, Larsson L. Evidence‐based strategies for preventing drug administration errors during anaesthesia. Anaesthesia. 2004; 59(5):493-504. [DOI:10.1111/j.1365-2044.2004.03670.x] [PMID]
- The American Society of Health-System Pharmacists. Pharmacists TASoH-S. The American Society of Health-System Pharmacists. 2016.
- Sen S, Chini EN, Brown MJ. Complications after unintentional intra-arterial injection of drugs: Risks, outcomes, and management strategies. Mayo Clinic Proceedings. 2005; 80(6):783-95. [DOI:10.4065/80.6.783] [PMID]
- Najafi A, Akbari H, Khajavi MR, Etezadi F. Inadvertent intrathecal injection of large dose magnesium sulfate. Saudi Journal of Anaesthesia. 2013; 7(4):464-6. [DOI:10.4103/1658-354X.121049] [PMID] [PMCID]
- Watterson LM, Morris RW, Westhorpe RN, Williamson JA. Crisis manage-ment during anaesthesia: Bradycardia. BMJ Quality & Safety. 2005; 14(1):156-63. [DOI:10.1136/qshc.2004.012856] [PMID] [PMCID]
- Salihoglu Z, Demiroluk S, Kose Y. Accidental subarachnoid injection of atracurium: A case report. Journal of Anesthesia. 2002; 16(1):72-4. [DOI:10.1007/s540-002-8097-y] [PMID]
- Cardone C, Szenohradszky J, Yost S, Bickler PE. Activation of brain acetylcholine receptors by neuromuscular blocking drugs: A possible mechanism of neurotoxicity. Anesthesiology. 1994; 80(5):1155-61. [DOI:10.1097/00000542-199405000-00025] [PMID]
- Zirak N, Soltani G, Ghomian N, Hasanpour MR, Mashayekhi Z. Inadvertent intrathe-cal injection of atracurium. Saudi Journal of Anaesthesia. 2011; 5(2):223-5. [DOI:10.4103/1658-354X.82811] [PMID] [PMCID]
- Kuvaki B, Özbilgin Ş, Küçük AB. Inadvertent intrathecal injection of atracurium. Austin Journal of Anesthesia and Analgesia. 2017; 5(1):1055-8. [DOI:10.26420/austinjanesthesiaanalgesia.2017.1055]
- Kessel G, Barker I. Leg ischemia in an infant following accidental intraarterial ad-ministration of atracurium treated with caudal anesthesia. Anesthesia. 1996; 51:1154-6. [DOI:10.1111/j.1365-2044.1996.tb15056.x] [PMID]
Type of Study: Case Report and Review of Literature |
Subject:
Anesthesiology
Received: 2019/03/13 | Accepted: 2019/08/28 | Published: 2020/01/1
Received: 2019/03/13 | Accepted: 2019/08/28 | Published: 2020/01/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |