Volume 8, Issue 1 (1-2020)
J. Pediatr. Rev 2020, 8(1): 47-52 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Mahajan N, Khatri A, Kumar P, Khanam S. Congenital Perineal Lipoma-like Lipoblastoma. J. Pediatr. Rev 2020; 8 (1) :47-52
URL: http://jpr.mazums.ac.ir/article-1-249-en.html
URL: http://jpr.mazums.ac.ir/article-1-249-en.html
1- Department of Pathology, Chacha Nehru Bal Chikitsalaya Hospital, New Delhi, India.
2- Department of Pathology, Chacha Nehru Bal Chikitsalaya Hospital, New Delhi, India. ,a.khatri2008@gmail.com
3- Department of Pediatric Surgery, Chacha Nehru Bal Chikitsalaya Hospital, New Delhi, India.
2- Department of Pathology, Chacha Nehru Bal Chikitsalaya Hospital, New Delhi, India. ,
3- Department of Pediatric Surgery, Chacha Nehru Bal Chikitsalaya Hospital, New Delhi, India.
Full-Text [PDF 922 kb]
(2423 Downloads)
| Abstract (HTML) (5740 Views)
Full-Text: (5691 Views)
1. Introduction
Adipocytic tumors like lipoma, angiolipoma, intramuscular lipoma, lipomatosis, etc. are common neoplasms of adults. However, they are rarely seen in the pediatric age group, too (1). The adipocytic tumor, which is commonly seen in children, especially less than 3 years of age, is Lipoblastoma (LB). LB accounts for less than 1% of childhood tumors, and it is more common in males (2). It is a benign lobulated soft tissue tumor comprising of hypocellular lobules of immature and mature adipocytes along with variable number of lipoblasts.
It has four histological subtypes, of which classical LB can easily be diagnosed by the presence of monovacuolated and multivacuolated lipoblasts. The difficulty arises when one has to search for these lipoblasts in the background of a classical lipoma (3). In such conditions, chances of misdiagnosing a lipoblastoma as classical lipoma is quite high, that may affect its management. We report a case of congenital lipoma-like lipoblastoma clinically presenting as an anal tag. It is the first case of this rare entity being reported in medical literature as a congenital mass in the perianal region.
2. Case Presentation
A 10-day-old male was admitted to the paediatric surgery Outpatient Department (OPD) with a mass in the perianal region since birth. It was not associated with pain, discharge, or enlarging. He was born by normal vaginal delivery at 39 weeks of gestation. He weighed 2850 g with Apgar scores of seven and eight at one and five minutes. On examination, the mass was non-tender, pedunculated, skin-colored, and measured 1.5x1.5x1cm. It was located at the margin of the anal opening (Figure 1a). A provisional clinical diagnosis of anal tag was made and advised excision because of parent’s apprehension. No radiological investigation was done as the swelling was superficial and pedunculated.
His biochemical and hematological results were within normal limits. Local excision was done and sent for histopathological examination. Grossly, we excised a skin-covered soft tissue mass measuring 1.2cm in diameter. The cut section was yellow and had a soft to firm consistency. Histopathological examination showed a polypoidal tissue lined by hyperkeratotic and acanthotic epidermis. The deep dermis showed a well-delineated moderately cellular lesion comprising of lobules of adipocytes in varying stages of maturation, several mature adipocytes, and few interspersed multivacuolated lipoblasts.
These lobules were separated by prominent fibrous septae with tiny proliferating vessels, focal myxoid change, and occasional inflammatory cells (Figure 1b). The lipoblasts were large, multivacuolated with a scalloped centrally placed normochromatic to hyperchromatic nucleus (Figure 1c). On immunohistochemistry, these cells expressed S100. Facilities for pleomorphic adenoma gene 1 (PLAG1) immunohistochemistry and cytogenetics were not available, and hence they were not performed. A final diagnosis of lipoma-like lipoblastoma was made. The patient did well postoperatively and showed no recurrence in the six months follow-up period.
3. Discussion and Review of Literature
Jaffe gave the term lipoblastoma in 1926 to describe a rare benign soft tissue tumor of embryonic white fat cells (4). It grows rapidly during infancy and early childhood. In contrast, classical lipomas are seen in adults and composed of mature fat cells with the absence of a rapid growth phase (5). Lipoblastoma, however, is exclusively restricted to pediatric population with majority cases diagnosed in the first 3 years of life with a male preponderance (2, 6).
Clinically, lipoblastoma can be of two types: well-encapsulated superficial subtype (more common) and diffuse poorly circumscribed lipoblastomatosis (2). The latter are usually deep-seated. The common sites of various LBs include limbs, trunk, retroperitoneum, head, and neck. The mediastinum, heart, lung, mesentery, omentum, scrotum, labia, axillary, inguinal and perineal regions are very uncommon sites for tumor (4). LB most commonly presents as a superficial painless progressive mass. Other symptoms depend on the site of involvement owing to their pressure effect like mediastinal and abdominal lipoblastoma, which may lead to airway and gastrointestinal obstructive symptoms, respectively.
Imaging has a limited role in superficial LB but is required for the deep-seated lesions. On ultrasonography, they appear as homogeneous hyperechoic masses with or without the presence of mixed echogenicity or fluid-filled spaces. Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) may be required for definite spread and also for differentiating between LB and lipoblastomatosis. The latter is poorly circumscribed, has infiltrative margins and shows less prominent fat component (6, 7).
Amidst the two modalities, CT scan identifies the presence of fat conclusively and also detects calcification and ossification which helps differentiate LB from teratomas, a pediatric tumor often seen at this site (7). MRI, in contrast, is usually helpful in follow-up and recurrent cases (4). A small amount of fat can also be seen in involuting hemangioma, but their characteristic clinical course usually helps in distinguishing them from LB. Liposarcoma is another differential for tumors in extremities and deep-seated locations and is difficult to differentiate on imaging alone. Age of the patient is an important clue, as liposarcoma is extremely rare in children.
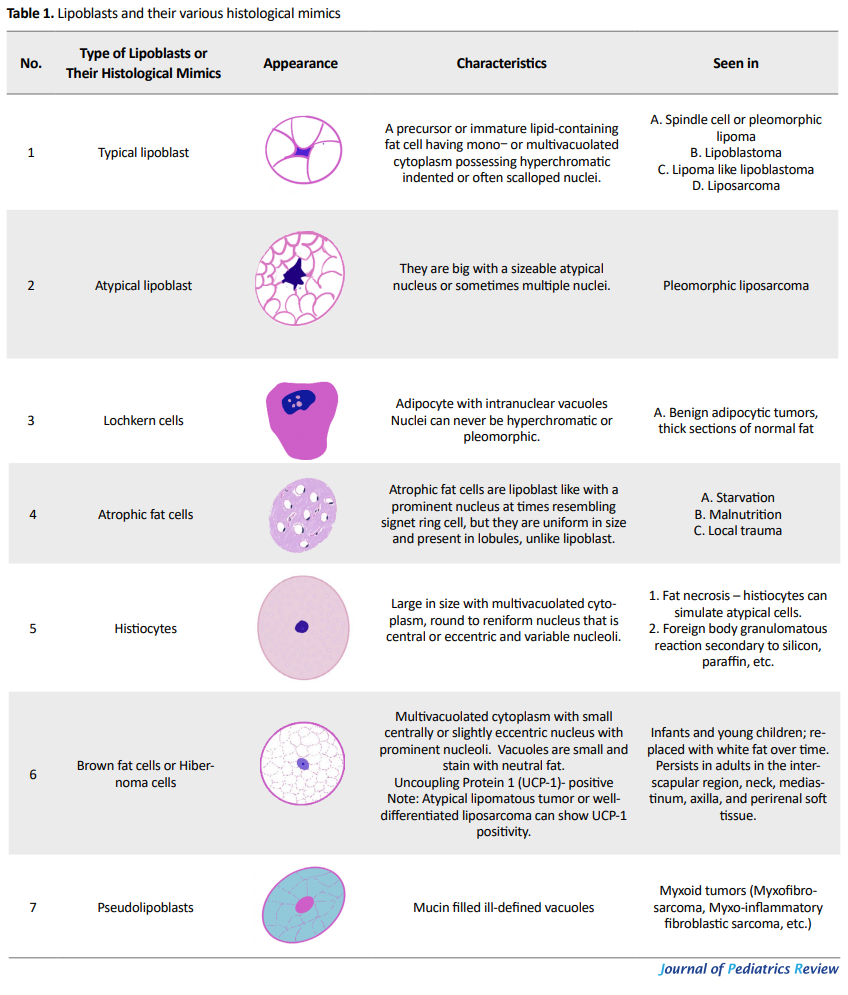
Histologically, LB is of four types: classic LB, myxoid LB, hibernoma-like LB, and lipoma-like LB. The classic LB shows adipocytes with spindle, stellate primitive mesenchymal cells with minimal myxoid component; myxoid LB shows abundant interstitial mucin, and hibernoma-like LB is composed of multivacuolated lipoblasts, few of which shows granular eosinophilic cytoplasm with the absence of myxoid component. The lipoma-like LB is mainly composed of mature adipocytes, with few lipoblasts and no myxoid component (1). Chung and Enzinger described infiltration into the surrounding skeletal muscle and lesser lobulation as important features differentiating lipoblastomatosis from typical lipoblastoma (8). Lipoblast is a unique mesenchymal cell that ranges in morphology from an immature fat cell resembling fibroblast to a mature fat cell with lipid droplets throughout its cytoplasm (9). There are many histomorphological mimics of lipoblasts which pose difficulty in making the correct diagnosis (Table 1) (9).
The clinical mimics of perianal tag include accessory scrotum, accessory labioscrotal fold, perineal lipoma, liposarcoma, teratoma, dermoid, hibernoma, and involuting hemangioma (7). These entities have characteristic histopathological features and can be differentiated easily. Accessory scrotum or labioscrotal fold shows smooth muscle bundles with interspersed dermal collagen. Classical lipoma shows an encapsulated mass composed of mature adipose tissue with thin septae and no atypia. Most teratomas and dermoid cysts show the presence of cystic areas or calcifications along with elements from all germ layers. The latter shows mainly ectodermal derivatives (7).
Hibernomas are commonly seen in 30-40 years of age, and most common sites involved are axilla followed by back. It is characterized by an organoid arrangement of large uniform cells with coarse granular to multivacuolated cytoplasm and a small central nucleus along with mature adipose tissue. As compared to lipoblastoma, hibernoma contains mainly brown fat and lacks lipoblasts (10). The involuting phase of hemangioma sometimes shows replacement of vascular element by mature adipose tissue. LB has been seen to be associated with PLAG1 gene abnormalities. This gene is located on chromosome 8q12.
The characteristic fusion of PLAG1- HAS2 (Hyaluronan synthase 2) has helped establish a correct diagnosis of LB in many difficult cases (1). The salient features of lipoma-like lipoblastoma composed mainly of mature adipose tissue with striking lobulation, few scattered lipoblasts, and abnormalities of PLAG1. There is usually no nuclear atypia or mitosis. Lipoma-like lipoblastoma or fat-rich lipoblastoma is an infrequent entity. It can be easily missed as a classical lipoma on histology; however, the presence of well-defined lobules and a meticulous search for lipoblasts can help establish diagnosis in these cases especially in the pediatric population (1).
LB, in general, has a rapid growth rate and a potential for local invasion. However, despite this feature, the prognosis is good. Various studies have reported the local recurrence rate of 0-25% (4). Unlike classical lipoblastoma, complete surgical excision with a wide margin is the management of choice of lipoma like lipoblastoma, as there is a risk of recurrence. However, it is not advised to do radical surgeries in cases of deep-seated lipoblastomas in an attempt to ensure complete resection as metastasis has not been reported so far (7).
4. Conclusion
Lipoma-like lipoblastoma can be seen as a congenital mass. An accurate diagnosis of lipoma-like lipoblastoma is essential for the appropriate management and requires awareness of this entity as probability of misdiagnosing it as a classical lipoma is quite high. Complete excision with wide margins is the treatment of choice in this lesion to prevent recurrence vis a vis classical lipoma which needs enucleation.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article. The participants were informed about the purpose of the research and its implementation stages; they were also assured about the confidentiality of their information; Moreover, They were allowed to leave the study whenever they wish, and if desired, the results of the research would be available to them.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors contribution's
All authors contributed in preparing this article.
Conflicts of interest
The authors declared no conflict of interest.
References
- Morerio C, Nozza P, Tassano E, Rosanda C, Granata C, Conte M, et al. Differential diagnosis of lipoma-like lipoblastoma. Pediatr Blood Cancer. 2009; 52(1):132-4. [DOI:10.1002/pbc.21747] [PMID]
- Kamal AF, Wiratnaya IGE, Hutagalung EU, Prasetyo M, Kodrat E, Widodo W, et al. Lipoblastoma and Lipoblastomatosis of the lower leg. Case Rep Orthop. 2014; 2014(582876):1-6. [DOI:10.1155/2014/582876] [PMID] [PMCID]
- Xu Y, Ogose A, Ariizumi T, Kawashima H, Hotta T, Li G, et al. Lipoma-like lipoblastoma arising from the femoral vein. Journal of Orthopaedic Science. 2011; 16(1):114-8. [DOI:10.1007/s00776-010-0001-7] [PMID]
- Kok KY, Telisinghe PU. Lipoblastoma: Clinical features, treatment, and outcome. World Journal of Surgery. 2010; 34(7):1517-22. [DOI:10.1007/s00268-010-0466-8] [PMID]
- Navarro OM, Laffan EE, Ngan BY. Pediatric soft-tissue tumors and pseudo-tumors: MR imaging features with pathologic correlation: Part 1. Imaging approach, pseudotumors, vascular lesions, and adipocytic tumors. Radiographics. 2009; 29(3):887-906. [DOI:10.1148/rg.293085168] [PMID]
- Bruyeer E, Lemmerling M, Poorten VV, Sciot R, Hermans R. Paediatric lipoblastoma in the head and neck: Three cases and review of literature. Cancer Imaging. 2012; 12(3):484-7. [DOI:10.1102/1470-7330.2012.0037] [PMID] [PMCID]
- Moholkar S, Sebire NJ, Roebuck DJ. Radiological-pathological correlation in lipoblastoma and lipoblastomatosis. Pediatric Radiology. 2006; 36(8):851-6. [DOI:10.1007/s00247-006-0175-5] [PMID]
- Chung EB, Enzinger FM. Benign lipoblastomatosis: An analysis of 35 cases. Cancer. 1973; 32(2):482-92. [DOI:10.1002/1097-0142(197308)32:23.0.CO;2-E]
- Hisaoka M. Lipoblast: Morphologic features and diagnostic value. Journal of UOEH. 2014; 36(2):115-21. [DOI:10.7888/juoeh.36.115] [PMID]
- Murphey MD, Carroll JF, Flemming DJ, Pope TL, Gannon FH, Kransdorf MJ. From the archives of the AFIP: Benign musculoskeletal lipomatous lesions. Radiographics. 2004; 24(5):1433-66. [DOI:10.1148/rg.245045120] [PMID]
Type of Study: Case Report and Review of Literature |
Subject:
Pathology
Received: 2019/07/25 | Accepted: 2019/08/18 | Published: 2020/01/1
Received: 2019/07/25 | Accepted: 2019/08/18 | Published: 2020/01/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |