Volume 8, Issue 1 (1-2020)
J. Pediatr. Rev 2020, 8(1): 15-22 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Motaharifard M S, Effatpanah M, Nejatbakhsh F. Nocturnal Enuresis in Children and Its Herbal Remedies in Medieval Persia: A Narrative Review. J. Pediatr. Rev 2020; 8 (1) :15-22
URL: http://jpr.mazums.ac.ir/article-1-222-en.html
URL: http://jpr.mazums.ac.ir/article-1-222-en.html
1- Department of Persian Medicine, School of Persian Medicine, Tehran University of Medical Sciences, Tehran, Iran.
2- School of Medicine, Ziaeian Hospital, International Campus, Tehran University of Medical Sciences, Tehran, Iran.
3- Department of Persian Medicine, School of Persian Medicine, Tehran University of Medical Sciences, Tehran, Iran. ,nejatbakhsh@tums.ac.ir
2- School of Medicine, Ziaeian Hospital, International Campus, Tehran University of Medical Sciences, Tehran, Iran.
3- Department of Persian Medicine, School of Persian Medicine, Tehran University of Medical Sciences, Tehran, Iran. ,
Full-Text [PDF 396 kb]
(2956 Downloads)
| Abstract (HTML) (6900 Views)
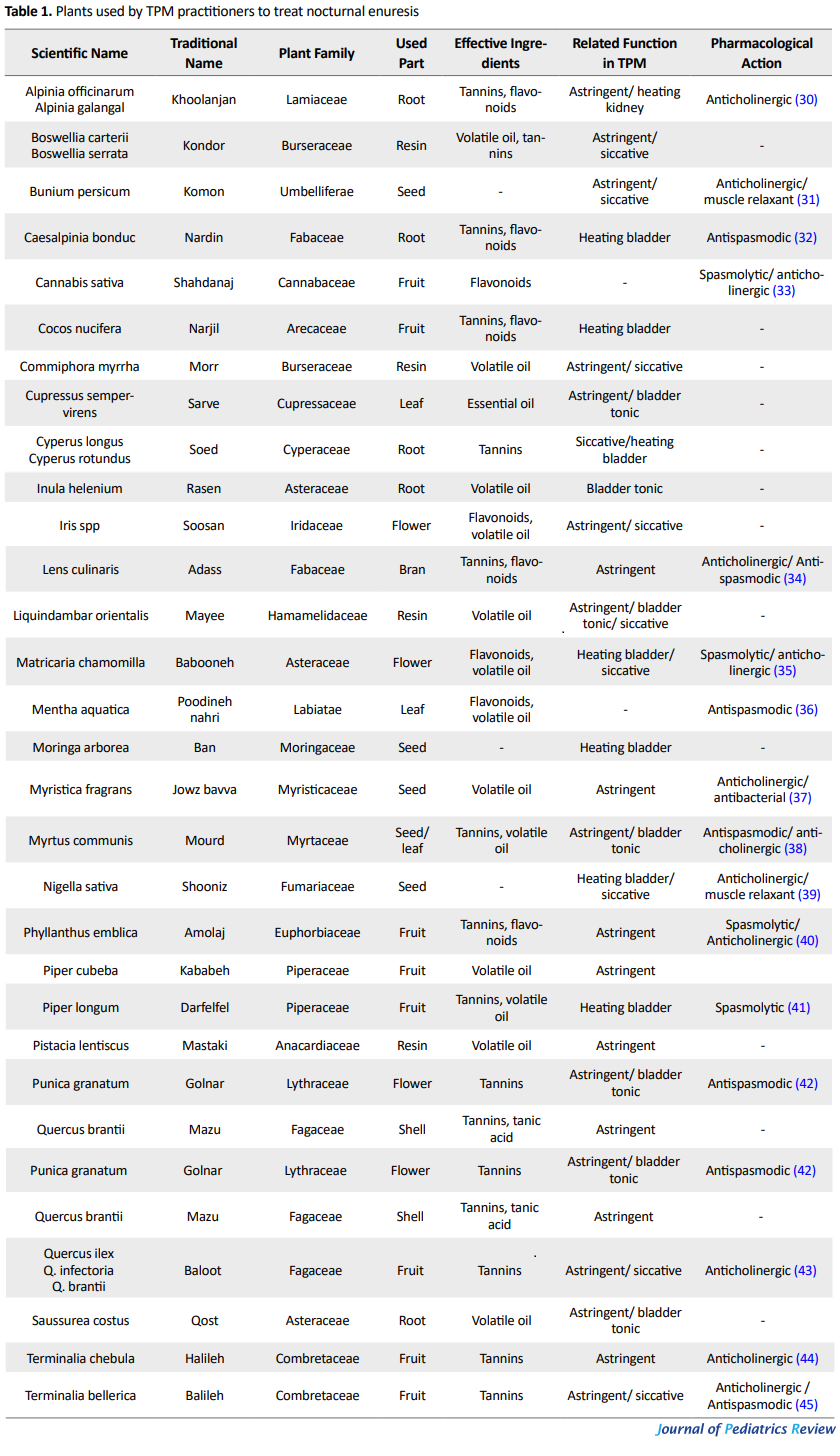
The specific mechanism of action of these herbs is unknown, but most of them have tannin content that strengthens the muscles. Tannins are astringent and can also be useful in protecting the kidneys. Reportedly, they have antibacterial effects and are used as antidiuretics for internal uses (25, 26). Besides, their flavonoids are well known for their antispasmodic activity that can have a beneficial role in enuresis treatment (27). Also some of these plants have essential or volatile oils which are possible to have anticholinergic activity (28). Certain drugs commonly prescribed for urinary incontinence, produce a direct antispasmodic action by inhibiting the muscarinic action of acetylcholine on smooth muscle and then relaxing the detrusor muscle (29). Table 1 presents medical plants that have also been investigated for this condition.
4. Discussion
One of the known forms of therapeutic application is anointing the bladder area with hot nature oil. Herbal oils are easily prepared and continued to be used as practical therapeutic interventions in ITM (46). Transdermal delivery is convenient and offers several advantages. They have been recently introduced in the medical literature for the treatment of detrusor muscle overactivity (47).
Nowadays herbalists suggest Hypericum perforatum, infusions of horsetail or corn silk (Zea mays), to be given through the day to encourage normal nervous control of the bladder but few published studies exist about their use (6, 48). There was no article related to our topic in Persian. There are few trial studies on complementary herbal therapies for NE, especially in children. Most of them have studied the effects of Chinese traditional herbs on children’s enuresis. In three trials, different preparations of Chinese medicinal herbs were compared with imipramine, and the herbs seemed to be better than imipramine both during and after the treatment (9). Some clinical trials assessed the efficacy and safety of “Suoquan” (a herbal medicine) used in traditional Korean and traditional Chinese medicine for the treatment of enuresis (49). “Yokukansan” is a Japanese traditional herbal prescription that is a candidate for the second-line therapy of nocturnal enuresis (50).
According to our search in scientific databases, only one clinical trial exists that confirms the effectiveness of medicinal plants listed in Table 1 on children’s enuresis. It is a double-blind, randomized clinical trial and concludes that the topical use of chamomile oil can decrease the episodes of enuresis in children compared with using a placebo (35). A few other studies have investigated these plants (listed in Table 1) for urological problems in adults. A study in India in 2014 showed that the combination of Boswellia serrata (Kondor) and Cyperus scariosus plus pelvic floor muscle training in stress incontinence in women of reproductive age was more effective than that in the control group (51). A double-blind placebo-controlled study showed that Saussurea costus (Qost) oil was effective on female urinary incontinence (52).
Enuresis is one of the frequently-seen problems during childhood, so, logically, it needs the most effective treatments. There are currently no specific medications to target incontinence symptoms without having side effects, so we need to find new medicines for the prevention or treatment of urinary incontinence. Herbal medicines have been broadly used in the treatment of a wide range of pediatric disorders such as NE and are considered safe and effective treatments. The purpose of this study was to investigate the opinions of Iranian practitioners about the herbal remedies for the treatment of NE in children.
A review of Rhazes’ opinion (854-925/935 AD), a genius Iranian physician, about NE, shows that medical practice in the past was comparable to our modern medicine yet tries avoiding the side effects in modern therapeutic approach (24). According to PM practices, the first step in NE treatment is to modify the lifestyle. Persian practitioners have introduced some natural remedies for this problem besides principles of lifestyle modification. In the present research, 29 plants have been extracted from ancient Persian documents which are supposed to be the most frequently-used herbs used for the treatment of NE in children. These medicinal herbs can be used alone or formulated with pharmaceutically acceptable compositions with a favorable delivery profile.
Most of these plants are warm and dry, which are recommended for cold and wet temperament diseases such as urinary incontinence. The definite mechanisms for the effect of these plants in treating NE have remained unknown. Based on the principles of TPM, the expected function of these medicinal plants are warming up the bladder by promoting venous circulation to the kidneys and bladder area, being siccative to remove waste from bladder and being astringent to improve bladder tone and strengthen kidneys and bladder.
5. Conclusion
In this review, we tried to connect TPM knowledge and current pharmacological data to identify new efficient drugs. Despite the extensive use of many of these herbs, little evidence supports their use, and proper randomized trials should be done to demonstrate their effectiveness. All traditional drugs and therapeutic approaches for using in our current medical practice should be evaluated and standardized with current standards of pharmaceutics and medical procedures.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors contribution's
Conceptualization, investigation, writing-original draft: Monireh Sadat Motaharifard; Methodology, writing-review & editing: Mohammad Effatpanah, Fatemeh Nejatbakhsh; Reading and approving the final manuscript: All authors.
Conflicts of interest
The authors declared no conflict of interests.
References
Full-Text: (3959 Views)
1. Context
Nocturnal Enuresis (NE) is defined as episodes of urinary incontinence during sleep in a child aged five years or more (1). The bedwetting must occur at least twice per week for at least 3 months or must have a negative impact on other important areas of functioning (2). Enuresis can be primary or secondary. Primary enuresis is diagnosed in a child who has never achieved nighttime dryness, while secondary enuresis is when the child has no enuresis for at least 6 months and starts up again. About (90%) of patients have primary enuresis (3). Prevalence of enuresis is approximately (5-10%) among 5 years old children, (1.5-5%) among 9-10 years old children, and about (1%) among people 15 years and older (2).
These figures may vary according to cultural, racial, and health variables among countries, and there is a slightly higher prevalence in boys (4). This disorder has a multifactorial etiology. Genetics, environmental factors (physical, neurologic, psychological factors) and other medical conditions have been implicated, so far (5). Children with NE may show signs of delayed maturation of the nervous system (6). Studies have suggested that detrusor muscle overactivity has an essential role in children with enuresis (7).
Although bedwetting is pathologically benign and has a high rate of spontaneous remission, it may affect the quality of life and self-esteem, which can be cured with successful treatment. Medical treatments include using anticholinergic drugs (with antispasmodic effects), smooth muscle relaxants, tricyclic antidepressants, and antidiuretics. Behavioral interventions involve using alarms, overlearning, scheduled wakening, star charts, reward systems, retention control training, and multidimensional behavioral treatments (8). Because of insufficient efficacy and significant side effects of the current interventions, many families are interested in complementary and integrative approaches (9).
Dating back to 1550 BC, a broad spectrum of alternative therapies have been used for the treatment of bedwetting (6). Today, different types of complementary and alternative medicines are being practiced in most parts of the world based on their availability and affordability. Hypnosis, acupuncture, chiropractic, diet (restricted foods), medicinal herbs, homeopathy, and traditional medicines, including Traditional Persian Medicine (TPM) are used to cure bedwetting (5). There is a lot of information in Iranian classic medical books about medicinal herbs used by pioneering practitioners for the treatment of enuresis in children. The present study aimed to introduce the most commonly used medicinal plants used in TPM for the treatment of nocturnal enuresis in children.
2. Evidence Acquisition
We reviewed eight original important textbooks of TPM; Qanun fi al-Tibb by Avicenna, Al Havi by Rhazes, Qarabadin-e-azam by Nazim Jahan, Exir-e-Azam by Nazim Jahan, Kholase al-Hekmah by Aghili Khorasani, Mufarrih al-Qulub by Arzani, Kamel al-sanaya al-tebbia by Ahwazi and Makhzan-ul-Adviah by Aghili Khorasani (10-17). In these books, the chapters containing information on NE were evaluated, and relevant data were collected, categorized, and analyzed. Then, the scientific names of the proposed plants were obtained using botanical textbooks of Popular Medicinal Plants of Iran and the annex of Makhzan-ul-Adviah (17-19).
Next, their active ingredients were evoked from the Physicians’ Desk Reference (PDR) for Herbal Medicines (20). We considered the scientific names of the plants in combination with “enuresis” OR “incontinency” and “children” OR “pediatric” as key words. Based on these key words, we established literature search in scientific databases of PubMed, Web of Science, Google Scholar, and some Iranian databases like SID and IranMedex. We tried to find out recent scientific documents in modern medicine to obtain any in vitro, animal, and clinical evidence related to NE in children to establish the relationship between traditional knowledge and current findings. The search was conducted on publications from all years until late 2018 and outputs were restricted to those completed studies published in English or Persian. The first author read and selected the related articles. The collected data from TPM books and modern sources were submitted to other authors; thus, all authors were involved in the process of analysis.
3. Results
NE is a well-known disorder mentioned in TPM. In 1472, Paulus Bagellardus of Padua published a book on diseases of children including one chapter entitled “on incontinence of urine and bedwetting”. He followed the Galenic doctrine of humours closely and mentioned the treatment of enuresis by contemporary Iranian physicians, including Rhazes and Avicenna (21). Avicenna (980‑1037 AD), the famous Iranian scientist, in his book “The Canon of Medicine” wrote that the most important cause of enuresis was “sterkha” meaning loosening of external sphincter’s muscular tone due to moisture in the muscle fibers. Loose muscle cannot contract strongly on the bladder’s neck, so it fails to prevent the involuntary outflow of urine (10).
Another cause of enuresis is bladder weakness due to coldness that decreases the intrinsic natural power of bladder to hold urine during sleep (22). From the perspective of TPM, children and elderly are two at-risk groups for urine incontinence (23). Children for two reasons are prone to enuresis: high humidity and wetness dominancy in their temperament and deeper sleep that prevents them from waking to urinate voluntarily. The wetness decreases when children grow up, so enuresis reduces (13).
In Persian Medicine (PM), lifestyle modification in addition to herbal, animal, and mineral medicines have been used to treat NE; however, most remedies have focused on medicinal herbs. Conservative management includes refraining from taking any beverages and diuretics at night, minimizing the amount of food consumed for dinner, avoiding heavy sleep, and waking up children frequently during the night (to ask them to urinate) (24). To resolve enuresis, strengthening the bladder and external sphincter by warming up the bladder and removing moisture from the external sphincter is necessary (14). For this purpose, TPM texts have mentioned many herbal remedies that are used in various forms like oral preparations, topical poultice, medicated oils, sitz baths, and fumigation. Table 1 presents these plants with their scientific name(s), plant family, type of application and related function(s) in alphabetic order.
Nocturnal Enuresis (NE) is defined as episodes of urinary incontinence during sleep in a child aged five years or more (1). The bedwetting must occur at least twice per week for at least 3 months or must have a negative impact on other important areas of functioning (2). Enuresis can be primary or secondary. Primary enuresis is diagnosed in a child who has never achieved nighttime dryness, while secondary enuresis is when the child has no enuresis for at least 6 months and starts up again. About (90%) of patients have primary enuresis (3). Prevalence of enuresis is approximately (5-10%) among 5 years old children, (1.5-5%) among 9-10 years old children, and about (1%) among people 15 years and older (2).
These figures may vary according to cultural, racial, and health variables among countries, and there is a slightly higher prevalence in boys (4). This disorder has a multifactorial etiology. Genetics, environmental factors (physical, neurologic, psychological factors) and other medical conditions have been implicated, so far (5). Children with NE may show signs of delayed maturation of the nervous system (6). Studies have suggested that detrusor muscle overactivity has an essential role in children with enuresis (7).
Although bedwetting is pathologically benign and has a high rate of spontaneous remission, it may affect the quality of life and self-esteem, which can be cured with successful treatment. Medical treatments include using anticholinergic drugs (with antispasmodic effects), smooth muscle relaxants, tricyclic antidepressants, and antidiuretics. Behavioral interventions involve using alarms, overlearning, scheduled wakening, star charts, reward systems, retention control training, and multidimensional behavioral treatments (8). Because of insufficient efficacy and significant side effects of the current interventions, many families are interested in complementary and integrative approaches (9).
Dating back to 1550 BC, a broad spectrum of alternative therapies have been used for the treatment of bedwetting (6). Today, different types of complementary and alternative medicines are being practiced in most parts of the world based on their availability and affordability. Hypnosis, acupuncture, chiropractic, diet (restricted foods), medicinal herbs, homeopathy, and traditional medicines, including Traditional Persian Medicine (TPM) are used to cure bedwetting (5). There is a lot of information in Iranian classic medical books about medicinal herbs used by pioneering practitioners for the treatment of enuresis in children. The present study aimed to introduce the most commonly used medicinal plants used in TPM for the treatment of nocturnal enuresis in children.
2. Evidence Acquisition
We reviewed eight original important textbooks of TPM; Qanun fi al-Tibb by Avicenna, Al Havi by Rhazes, Qarabadin-e-azam by Nazim Jahan, Exir-e-Azam by Nazim Jahan, Kholase al-Hekmah by Aghili Khorasani, Mufarrih al-Qulub by Arzani, Kamel al-sanaya al-tebbia by Ahwazi and Makhzan-ul-Adviah by Aghili Khorasani (10-17). In these books, the chapters containing information on NE were evaluated, and relevant data were collected, categorized, and analyzed. Then, the scientific names of the proposed plants were obtained using botanical textbooks of Popular Medicinal Plants of Iran and the annex of Makhzan-ul-Adviah (17-19).
Next, their active ingredients were evoked from the Physicians’ Desk Reference (PDR) for Herbal Medicines (20). We considered the scientific names of the plants in combination with “enuresis” OR “incontinency” and “children” OR “pediatric” as key words. Based on these key words, we established literature search in scientific databases of PubMed, Web of Science, Google Scholar, and some Iranian databases like SID and IranMedex. We tried to find out recent scientific documents in modern medicine to obtain any in vitro, animal, and clinical evidence related to NE in children to establish the relationship between traditional knowledge and current findings. The search was conducted on publications from all years until late 2018 and outputs were restricted to those completed studies published in English or Persian. The first author read and selected the related articles. The collected data from TPM books and modern sources were submitted to other authors; thus, all authors were involved in the process of analysis.
3. Results
NE is a well-known disorder mentioned in TPM. In 1472, Paulus Bagellardus of Padua published a book on diseases of children including one chapter entitled “on incontinence of urine and bedwetting”. He followed the Galenic doctrine of humours closely and mentioned the treatment of enuresis by contemporary Iranian physicians, including Rhazes and Avicenna (21). Avicenna (980‑1037 AD), the famous Iranian scientist, in his book “The Canon of Medicine” wrote that the most important cause of enuresis was “sterkha” meaning loosening of external sphincter’s muscular tone due to moisture in the muscle fibers. Loose muscle cannot contract strongly on the bladder’s neck, so it fails to prevent the involuntary outflow of urine (10).
Another cause of enuresis is bladder weakness due to coldness that decreases the intrinsic natural power of bladder to hold urine during sleep (22). From the perspective of TPM, children and elderly are two at-risk groups for urine incontinence (23). Children for two reasons are prone to enuresis: high humidity and wetness dominancy in their temperament and deeper sleep that prevents them from waking to urinate voluntarily. The wetness decreases when children grow up, so enuresis reduces (13).
In Persian Medicine (PM), lifestyle modification in addition to herbal, animal, and mineral medicines have been used to treat NE; however, most remedies have focused on medicinal herbs. Conservative management includes refraining from taking any beverages and diuretics at night, minimizing the amount of food consumed for dinner, avoiding heavy sleep, and waking up children frequently during the night (to ask them to urinate) (24). To resolve enuresis, strengthening the bladder and external sphincter by warming up the bladder and removing moisture from the external sphincter is necessary (14). For this purpose, TPM texts have mentioned many herbal remedies that are used in various forms like oral preparations, topical poultice, medicated oils, sitz baths, and fumigation. Table 1 presents these plants with their scientific name(s), plant family, type of application and related function(s) in alphabetic order.
The specific mechanism of action of these herbs is unknown, but most of them have tannin content that strengthens the muscles. Tannins are astringent and can also be useful in protecting the kidneys. Reportedly, they have antibacterial effects and are used as antidiuretics for internal uses (25, 26). Besides, their flavonoids are well known for their antispasmodic activity that can have a beneficial role in enuresis treatment (27). Also some of these plants have essential or volatile oils which are possible to have anticholinergic activity (28). Certain drugs commonly prescribed for urinary incontinence, produce a direct antispasmodic action by inhibiting the muscarinic action of acetylcholine on smooth muscle and then relaxing the detrusor muscle (29). Table 1 presents medical plants that have also been investigated for this condition.
4. Discussion
One of the known forms of therapeutic application is anointing the bladder area with hot nature oil. Herbal oils are easily prepared and continued to be used as practical therapeutic interventions in ITM (46). Transdermal delivery is convenient and offers several advantages. They have been recently introduced in the medical literature for the treatment of detrusor muscle overactivity (47).
Nowadays herbalists suggest Hypericum perforatum, infusions of horsetail or corn silk (Zea mays), to be given through the day to encourage normal nervous control of the bladder but few published studies exist about their use (6, 48). There was no article related to our topic in Persian. There are few trial studies on complementary herbal therapies for NE, especially in children. Most of them have studied the effects of Chinese traditional herbs on children’s enuresis. In three trials, different preparations of Chinese medicinal herbs were compared with imipramine, and the herbs seemed to be better than imipramine both during and after the treatment (9). Some clinical trials assessed the efficacy and safety of “Suoquan” (a herbal medicine) used in traditional Korean and traditional Chinese medicine for the treatment of enuresis (49). “Yokukansan” is a Japanese traditional herbal prescription that is a candidate for the second-line therapy of nocturnal enuresis (50).
According to our search in scientific databases, only one clinical trial exists that confirms the effectiveness of medicinal plants listed in Table 1 on children’s enuresis. It is a double-blind, randomized clinical trial and concludes that the topical use of chamomile oil can decrease the episodes of enuresis in children compared with using a placebo (35). A few other studies have investigated these plants (listed in Table 1) for urological problems in adults. A study in India in 2014 showed that the combination of Boswellia serrata (Kondor) and Cyperus scariosus plus pelvic floor muscle training in stress incontinence in women of reproductive age was more effective than that in the control group (51). A double-blind placebo-controlled study showed that Saussurea costus (Qost) oil was effective on female urinary incontinence (52).
Enuresis is one of the frequently-seen problems during childhood, so, logically, it needs the most effective treatments. There are currently no specific medications to target incontinence symptoms without having side effects, so we need to find new medicines for the prevention or treatment of urinary incontinence. Herbal medicines have been broadly used in the treatment of a wide range of pediatric disorders such as NE and are considered safe and effective treatments. The purpose of this study was to investigate the opinions of Iranian practitioners about the herbal remedies for the treatment of NE in children.
A review of Rhazes’ opinion (854-925/935 AD), a genius Iranian physician, about NE, shows that medical practice in the past was comparable to our modern medicine yet tries avoiding the side effects in modern therapeutic approach (24). According to PM practices, the first step in NE treatment is to modify the lifestyle. Persian practitioners have introduced some natural remedies for this problem besides principles of lifestyle modification. In the present research, 29 plants have been extracted from ancient Persian documents which are supposed to be the most frequently-used herbs used for the treatment of NE in children. These medicinal herbs can be used alone or formulated with pharmaceutically acceptable compositions with a favorable delivery profile.
Most of these plants are warm and dry, which are recommended for cold and wet temperament diseases such as urinary incontinence. The definite mechanisms for the effect of these plants in treating NE have remained unknown. Based on the principles of TPM, the expected function of these medicinal plants are warming up the bladder by promoting venous circulation to the kidneys and bladder area, being siccative to remove waste from bladder and being astringent to improve bladder tone and strengthen kidneys and bladder.
5. Conclusion
In this review, we tried to connect TPM knowledge and current pharmacological data to identify new efficient drugs. Despite the extensive use of many of these herbs, little evidence supports their use, and proper randomized trials should be done to demonstrate their effectiveness. All traditional drugs and therapeutic approaches for using in our current medical practice should be evaluated and standardized with current standards of pharmaceutics and medical procedures.
Ethical Considerations
Compliance with ethical guidelines
All ethical principles were considered in this article.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors contribution's
Conceptualization, investigation, writing-original draft: Monireh Sadat Motaharifard; Methodology, writing-review & editing: Mohammad Effatpanah, Fatemeh Nejatbakhsh; Reading and approving the final manuscript: All authors.
Conflicts of interest
The authors declared no conflict of interests.
References
- Nevéus T, von Gontard A, Hoebeke P, Hjälmås K, Bauer S, Bower W, et al. The standardization of terminology of lower urinary tract function in children and adolescents: Report from the standardisation committee of the international children’s continence society. The Journal of Urology. 2006; 176(1):314-24. [DOI:10.1016/S0022-5347(06)00305-3]
- Brown ML, Pope AW, Brown EJ. Treatment of primary nocturnal enuresis in children: A review. Child. 2011; 37(2):153-60. [DOI:10.1111/j.1365-2214.2010.01146.x] [PMID]
- Hadinezhad Makrani A, Moosazadeh M, Nasehi M, Abedi G, Afshari M, Farshidi F, et al. Prevalence of enuresis and its related factors among children in Iran: A systematic review and meta-analysis. International Journal of Pediatrics. 2015; 3(6.1):995-1004.
- Safarinejad MR. Prevalence of nocturnal enuresis, risk factors, associated familial factors and urinary pathology among school children in Iran. Journal of Pediatric Urology. 2007; 3(6):443-52. [DOI:10.1016/j.jpurol.2007.06.001] [PMID]
- Adams D, Vohra S. Complementary, holistic, and integrative medicine: Nocturnal enuresis. Pediatrics in Review/American Academy of Pediatrics. 2009; 30(10):396-400. [DOI:10.1542/pir.30-10-396] [PMID]
- Culbert TP, Banez GA. Wetting the bed: Integrative approaches to nocturnal enuresis. Explore. 2008; 4(3):215-20. [DOI:10.1016/j.explore.2008.02.014] [PMID]
- Yeung C, Chiu H, Sit F. Bladder dysfunction in children with refractory monosymptomatic primary nocturnal enuresis. The Journal of Urology. 1999; 162(3):1049-54. [DOI:10.1016/S0022-5347(01)68062-5] [PMID]
- Caldwell PH, Sureshkumar P, Wong WC. Tricyclic and related drugs for nocturnal enuresis in children. The Cochrane Database of Systematic Reviews. 2016; 2016(1):CD002117. [DOI:10.1002/14651858.CD002117.pub2] [PMID]
- Huang T, Shu X, Huang YS, Cheuk DK. Complementary and miscellaneous interventions for nocturnal enuresis in children. The Cochrane Database of Systematic Reviews. 2011; 2011(12):CD005230. [DOI:10.1002/14651858.CD005230.pub2]
- Institute of Manuscripts, of Azerbaijan National Academy of Sciences. al-Qanun fi al-Tibb. Baku: Institute of Manuscripts of Azerbaijan National Academy of Sciences; 2005.
- Institute of Manuscripts, of Azerbaijan National Academy of Sciences. Al-Hawi fi al-tibb. Baku: Institute of Manuscripts of Azerbaijan National Academy of Sciences; 2002.
- Nazim Jahan MA. [(Qarabadin (azam) (Persian)]. Tehran: Iran University of Medical Sciences 2004.
- Azamkhan M. [Exir-e-Azam (Persian)]. Tehran: Research Institute for Islamic and Complementary Medicine; 2009.
- Aghili Khorasani MH. [Revelations-al-hekamah (Persian)]. Qom: Research Institute for Islamic & Complementary Medicine; 2006.
- Arzani MA. [Mufarrih al-qulub (Persian)]. Tehran: Almaee publications; 2012.
- Majoosi Ahvazi A. [Kamel al-sanaya al-tebbia (Arabic)]. Tehran: Institute of Natural Medicine’s Revival; 2008.
- Aghili Khorasani MH. [Makhzan-ol Advieh (Persian)]. Tehran: Tehran University of Medical Sciences; 1992.
- Amin Gh. [The most common medicinal plants of Iran (Persian)]. Tehran: Tehran University of Medical Sciences; 2005.
- Mozaffarian V. [A dictionary of Iranian plant names (Persian)]. Tehran: Farhangmoaser; 1996.
- Healthcare T. PDR for Herbal Medicines. Toronto: Thomson Reuters Corporation; 2007.
- Salmon MA. An historical account of nocturnal enuresis and its treatment. Proceedings of the Royal Society of Medicine. 1975; 68(7):443-5. [DOI:10.1177/003591577506800726] [PMID] [PMCID]
- Nojavan F, Ghanbari Z, Minaee M, Sharifi H. [Enuresis of children from the perspective of Iranian traditional medicine (Persian)]. Iranian Journal of Public Health. 2016; 45(3):407-8.
- Nojavan F, Sharifi H, Ghanbari Z, Kamalinejad M, Mokaberinejad R, Emami M. [Causes and risk factors of urinary incontinence: Avicenna’s point of view vs. contemporary findings (Persian)]. Urology Journal. 2015; 12(1):1995-8.
- Ashtiyani SC, Shamsi M, Cyrus A, Tabatabayei SM. Rhazes, a genius physician in the diagnosis and treatment of nocturnal enuresis in medical history. Iranian Red Crescent Medical Journal. 2013; 15(8):633-8. [DOI:10.5812/ircmj.5017] [PMID] [PMCID]
- Ashok PK, Upadhyaya K. Tannins are astringent. Journal of Pharmacognosy and Phytochemistry. 2012; 1(3):45-50.
- Agusti J, Carlos L. Pharmaceutical composition for treating urinary incontinence and enuresis. Geneva: World Intellectual Property Organization; 2016.
- Gilani AH, Khan Au, Ghayur MN, Ali SF, Herzig JW. Antispasmodic effects of rooibos tea (aspalathus linearis) is mediated predominantly through K+‐channel activation. Basic & Clinical Pharmacology & Toxicology. 2006; 99(5):365-73. [DOI:10.1111/j.1742-7843.2006.pto_507.x] [PMID]
- Oh M, Houghton P, Whang W, Cho J. Screening of Korean herbal medicines used to improve cognitive function for anti-cholinesterase activity. Phytomedicine. 2004; 11(6):544-8. [DOI:10.1016/j.phymed.2004.03.001] [PMID]
- Seipel TA, Biologic Health Solutions Pty Ltd. Herbal compositions for the prevention or treatment of urinary incontinence and overactive bladder. Savannah: United States Patent; 2008.
- Köse LP, Gülçin İ, Gören AC, Namiesnik J, Martinez-Ayala AL, Gorinstein S. LC-MS/MS analysis, antioxidant and anticholinergic properties of galanga (alpinia officinarum hance) rhizomes. Industrial Crops and Products. 2015; 74:712-21. [DOI:10.1016/j.indcrop.2015.05.034]
- Boskabady MH, Moghaddas A. Antihistaminic effect of Bunium persicum on Guinea pig tracheal chains. Iranian BioMedical Journal. 2004; 8(3):149-55.
- Singh V, Raghav PK. Review on pharmacological properties of Caesalpinia bonduc L. International Journal of Medicinal and Aromatic Plants. 2012; 2(3):514-30.
- Brady C, DasGupta R, Dalton C, Wiseman O, Berkley K, Fowler C. An open-label pilot study of cannabis-based extracts for bladder dysfunction in advanced multiple sclerosis. Multiple Sclerosis. 2004; 10(4):425-33. [DOI:10.1191/1352458504ms1063oa] [PMID]
- Khan M, Khan A, Gilani A. Pharmacological basis for medicinal use of Lens culinaris in gastrointestinal and respiratory disorders. Phytotherapy Research. 2014; 28(9):1349-58. [DOI:10.1002/ptr.5136] [PMID]
- Sharifi H, Minaie MB, Qasemzadeh MJ, Ataei N, Gharehbeglou M, Heydari M. Topical use of Matricaria Recutita l (Chamomile) oil in the treatment of monosymptomatic enuresis in children: A double-blind randomized controlled trial. Journal of Evidence-Based Complementary & Alternative Medicine. 2017; 22(1):12-7. [DOI:10.1177/2156587215608989] [PMID] [PMCID]
- Andro AR, Boz I, Zamfirache MM, Burzo I. Chemical composition of essential oils from Mentha aquatica L. at different moments of the ontogenetic cycle. Journal of Medicinal Plant Research. 2013; 7(9):470-3.
- Lee JY, Park W. Anti-inflammatory effect of myristicin on RAW 264.7 macrophages stimulated with polyinosinic-polycytidylic acid. Molecules. 2011; 16(8):7132-42. [DOI:10.3390/molecules16087132] [PMID] [PMCID]
- Aleksic V, Knezevic P. Antimicrobial and antioxidative activity of extracts and essential oils of Myrtus communis L. Microbiological Research. 2014; 169(4):240-54. [DOI:10.1016/j.micres.2013.10.003] [PMID]
- Boskabady MH, Shirmohammadi B, Jandaghi P, Kiani S. Possible mechanism(s) for relaxant effect of aqueous and macerated extracts from Nigella sativa on tracheal chains of guinea pig. BMC Pharmacology. 2004; 4:3. [DOI:10.1186/1471-2210-4-3] [PMID] [PMCID]
- Mehmood MH, Siddiqi HS, Gilani AH. The antidiarrheal and spasmolytic activities of Phyllanthus emblica are mediated through dual blockade of muscarinic receptors and Ca2+ channels. Journal of Ethnopharmacology. 2011; 133(2):856-65. [DOI:10.1016/j.jep.2010.11.023] [PMID]
- Zaveri M, Khandhar A, Patel S, Patel A. Chemistry and pharmacology of Piper longum L. International Journal of Pharmaceutical Sciences Review and Research. 2010; 5(1):67-76.
- Ahangarpour A, Heidari R, Abdolahzadeh M, Oroojan AA. Antispasmodic effects of aqueous and Hydroalcoholic Punica granatum flower extracts on the uterus of non-pregnant rats. Journal of Reproduction & Infertility. 2012; 13(3):138-42. [PMID] [PMCID]
- Dar MS, Ikram M, Fakouhi T. Pharmacology of quercus infectoria. Journal of Pharmaceutical Sciences. 1976; 65(12):1791-4. [DOI:10.1002/jps.2600651224] [PMID]
- Swamy P, Prasad V, Krishna B, Rao T, Kumar L, Rao G. In vitro anticholinergic activity of selected culinary spices on sheep airway smooth muscle. International Journal of Recent Scientific Research. 2013; 4(5):649-53.
- Gilani AH, Khan AU, Ali T, Ajmal S. Mechanisms underlying the antispasmodic and bronchodilatory properties of Terminalia bellerica fruit. Journal of Ethnopharmacology. 2008; 116(3):528-38. [DOI:10.1016/j.jep.2008.01.006] [PMID]
- Hamedi A, Zarshenas MM, Sohrabpour M, Zargaran A. Herbal medicinal oils in traditional Persian medicine. Pharmaceutical Biology. 2013; 51(9):1208-18. [DOI:10.3109/13880209.2013.777462] [PMID]
- MacDiarmid SA. The evolution of transdermal/topical overactive bladder therapy and its benefits over oral therapy. Reviews in Obstetrics and Gynecology. 2009; 2(2):116-21. [PMID] [PMCID]
- Rafsanjany N, Hensel A. Extract of maydis stigma (Zea mays L.) inhibits the adhesion of uropathogenic Escherichia coli (UPEC) to human bladder cells. Planta Medica. 2013; 79(13):PI88. [DOI:10.1055/s-0033-1352177]
- Lee YB, Lee JA, Jang S, Lee HL. Herbal medicine (Suoquan) for treating nocturnal enuresis: A protocol for a systematic review of randomized controlled trials. Medicine. 2018; 97(17):e0391. [DOI:10.1097/MD.0000000000010391] [PMID] [PMCID]
- Ohtomo Y, Umino D, Takada M, Niijima S, Fujinaga S, Shimizu T. Traditional Japanese medicine, Yokukansan, for the treatment of nocturnal enuresis in children. Pediatrics inTernational. 2013; 55(6):737-40. [DOI:10.1111/ped.12158] [PMID]
- Rangaswamy PA, Sultana A, Rahman K, Nagapattinam S. Efficacy of Boswellia serrata L. and Cyperus scariosus L. plus pelvic floor muscle training in stress incontinence in women of reproductive age. Complementary Therapies in Clinical Practice. 2014; 20(4):230-6. [DOI:10.1016/j.ctcp.2014.08.003] [PMID]
- Niktabe Z, Eftekhaar T, Mirabzadeh Ardakani M, Yekaninejad MS, Shirbeigi L, Ebadi N, et al. Efficacy of Saussurea costus (qost) oil as an Iranian traditional medicine product on female urinary incontinence; double blinded randomized clinical trial. Research Journal of Pharmacognosy. 2018; 5(3):47-55. [DOI:10.22127/RJP.2018.64876]
Type of Study: Narrative Review |
Subject:
Traditional Medicine
Received: 2019/01/3 | Accepted: 2019/06/1 | Published: 2020/01/1
Received: 2019/01/3 | Accepted: 2019/06/1 | Published: 2020/01/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |